 Call Us
+91 - 9840036061
Call Us
+91 - 9840036061
 Mail Us
[email protected]
Mail Us
[email protected]
 Office Hours
Monday to Saturday: 10.00 AM - 9.00 PM
Sunday: 10.00 AM - 5.00 PM
Office Hours
Monday to Saturday: 10.00 AM - 9.00 PM
Sunday: 10.00 AM - 5.00 PM
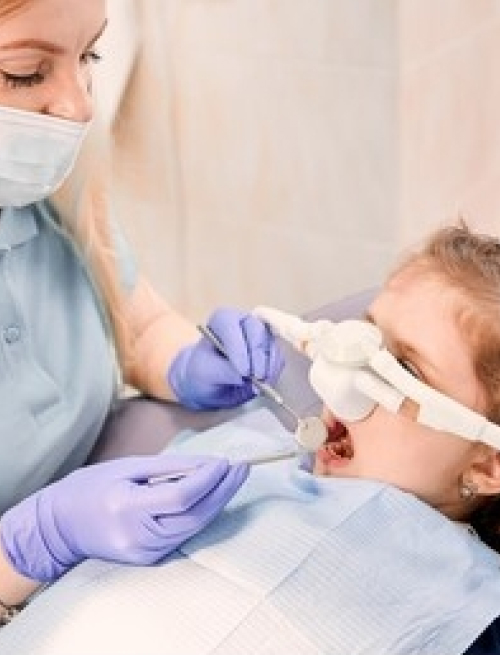
Sedation dentistry
What is sedation dentistry?
Sedation dentistry helps you feel calm, relaxed and at ease during dental procedures. It’s a moderate level of sedation, where you’re still awake but feeling very carefree. It’s sometimes called conscious sedation dentistry or “twilight sleep” because it creates a state of short-term amnesia (forgetfulness) where you experience insensitivity to pain without the loss of consciousness.
Who needs sedation dentistry?
People of all ages can benefit from sedation dentistry, including children. Dentists often recommend this option for those with:
Dental anxiety
A fear of visiting the dentist.
Sensitive gag reflex.
A fear of needles.
Extreme teeth sensitivity.
Feelings of claustrophobia while in the dental chair.
Decreased sensitivity to local anesthesia.
Difficulty controlling movements.
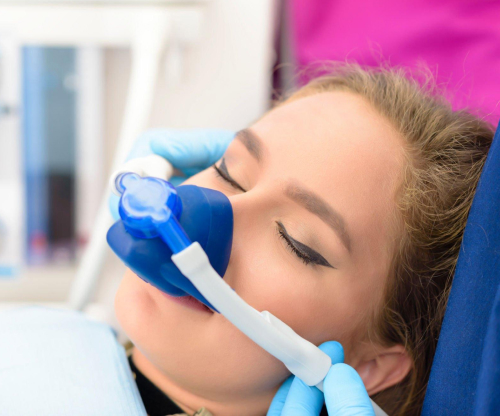
What types of sedation are used in dentistry?
There are varying levels of sedation dentistry based on your unique needs. Factors include your level of anxiety, the length of your procedure, your health history and personal preferences. The most common types of sedation dentistry include nitrous oxide, oral conscious sedation and intravenous (IV) sedation.
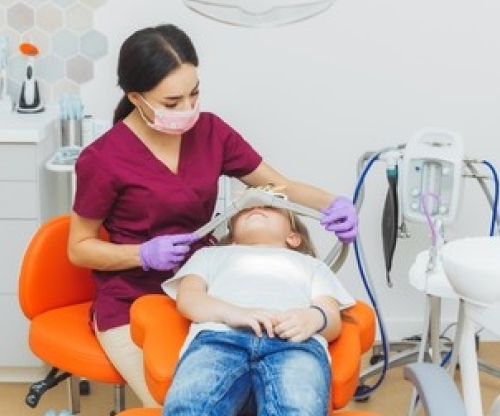
Nitrous oxide
Nitrous oxide is commonly known as “laughing gas.” You inhale nitrous oxide through a mask or nosepiece, and calming effects begin within three to five minutes. Your dentist controls the amount of sedation you receive and adjusts dosages accordingly throughout your procedure. Once your treatment is over, your dentist gives you pure oxygen to flush the nitrous oxide out of your system. Because the laughing gas leaves your system so quickly, you’ll be able to drive yourself home after the procedure.
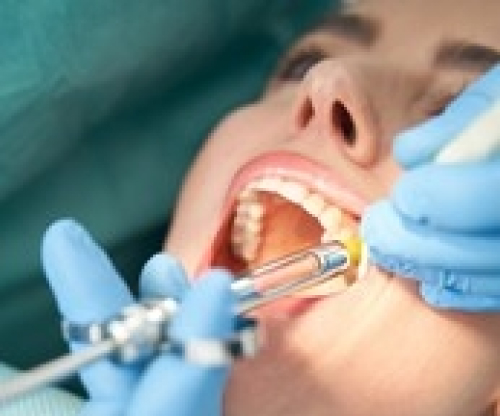
Oral conscious sedation
With oral conscious sedation, your dentist gives you sedative medication (usually in pill form) about an hour before your procedure begins. Most dentists use triazolam, which is in the diazepam family. But your dentist might use other medications. Dentists often used liquid sedation in pediatric dentistry, such as midazolam oral syrup.
Oral sedation makes you relax, and you may even fall asleep. But you’ll still be able to communicate with your dentist if necessary, and you’ll be awaken with a gentle nudge. Because oral sedation temporarily affects your memory and motor skills, you’ll need a friend or family member to drive you home after your procedure.
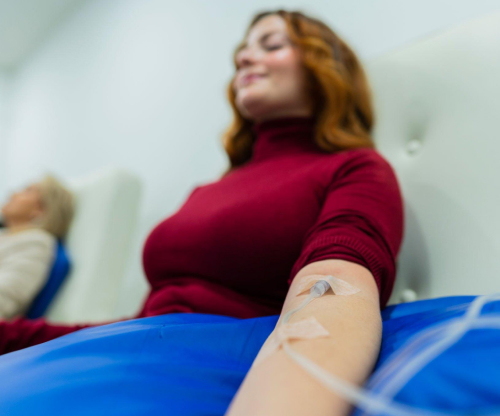
Intravenous (IV) sedation
IV sedation dentistry is the deepest form of conscious sedation available in a dental office setting. Your healthcare provider delivers sedative medications directly to your bloodstream through an IV line. During your procedure, your dentist monitors your heart rate, blood pressure and oxygen levels. They can adjust your dosage at any point and can use reversal medications if necessary. Most people who receive IV sedation dentistry fall asleep and have little to no memory of their treatment when they wake up. This option is best for people with severe dental anxiety or those who are undergoing lengthy procedures.
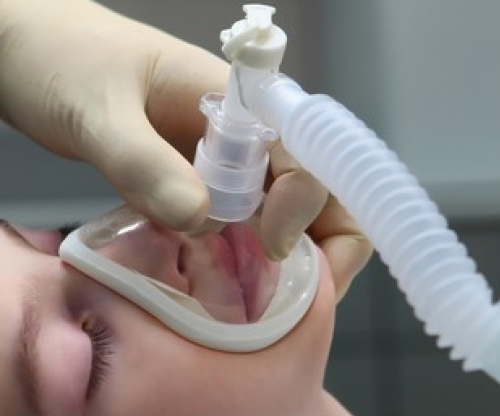
Is general anesthesia ever used in dentistry?
Yes, in some cases general anesthesia procedures are carried in a hospital may be necessary when treating young children, adults with special needs or people with severe dental anxiety. General anesthesia is a type of unconscious sedation. In other words, you’ll be completely unconscious during the procedure. To provide general anesthesia, your dentist must have advanced, specialized training. In most cases, an anesthesiologist provides this type of anesthesia.
Procedure Details
-
You’ll talk with your dentist about sedation options during your initial consultation. They’ll discuss your health history and ask about any medications or supplements you’re taking. Once they’ve gathered all the necessary information, they’ll make sedation recommendations based on your specific needs.
-
In most cases, you shouldn’t eat or drink anything for at least six hours before your dental appointment. Unless otherwise noted by your dentist, you should take all routine medications without interruption.
-
Be sure to tell your dentist if you’re taking any blood thinners. They may ask you to skip these medications for a few days leading up to your procedure.
-
Your dentist gives you sedative medications before beginning your procedure. You’ll still receive local anesthetic to numb your teeth and gums, but your dentist usually does this once you’re already feeling comfortable from the sedatives.
-
Unless you choose nitrous oxide as your sedation option, you’ll need a trusted friend or family member to drive you home after your appointment. You should go straight home and rest while the sedative medication wears off.
-
Never take a taxi or rideshare home after sedation dentistry. You’ll need a trusted and familiar person to help you. Before leaving you alone, your driver should make sure you’re resting comfortably in bed or on your couch.
Risks / Benefits
-
Sedation dentistry eases anxieties and phobias, helping you remain calm and comfortable during dental procedures. Because your dentist can often work faster when you’re under sedation, it can result in fewer appointments. Finally, many people have so much dental anxiety that they avoid going to the dentist altogether. Sedation dentistry helps you feel more comfortable so you can receive the care you need and deserve.
-
Sedation dentistry is typically safe when administered by a licensed healthcare provider. However, there’s a small risk of complications. Possible short-term risks include:
-
Lingering drowsiness.
-
Can be difficult to predict the effect of oral sedation medications.
-
Dry mouth (xerostomia).
-
Nausea and vomiting.
-
Headaches.
-
Bruising from the IV.
-
It can also be difficult to predict the effect of oral sedation medications. Rarely, people may have an allergic reaction. There are drugs available that can counteract these issues.
-
Sedation dentistry is safe for kids. But as a parent, it can still be scary when your child takes unfamiliar medications. Child sedation dentistry side effects are usually short-lived, but they can include:
-
Irritability.
-
Snoring.
-
Fever.
-
Nausea and vomiting.
-
Sometimes, your child can be slow to wake after sedation. If this happens, your dentist will monitor your child until they’re ready to go home. These side effects are normal and should go away on their own in a day or two. If you have specific questions or concerns, call your dentist.
-
Generally, sedation dentistry isn’t recommended for people who are pregnant because some sedative medications can affect fetal development. Nitrous oxide may be given during the second trimester in some cases. But overall, most dentists wait until after pregnancy to administer sedation dentistry.
